Roger, my father, is 59 years old and has been married to my mom, Jodi, for 35 years. He served in the Air Force for 20 years and transitioned to civilian telecommunications work in Soldotna in the early 2000s. He retired from that job around the beginning of October 2020. When the pandemic hit in March of 2020, my parents took it seriously. Since I work in public health, I regularly sent them any updated COVID-19 information because my father is susceptible to pneumonia, and I wanted to keep my parents up to date with facts from valid and reputable sources.
In mid-November Roger started to get cold-like symptoms. Since my parents had been cautious with masking and distancing, I asked them questions about their social behaviors. They had both recently spent time with the pastor of their church. Not long after, their pastor informed my parents that he had tested positive for COVID-19. It had just been the three of them meeting together, but Roger had removed his mask to drink coffee. That’s all it had taken. Roger was now experiencing chills, a stuffy nose, fever, and digestive issues. Jodi’s symptoms followed shortly after.
Roger initially thought it was a cold or possibly flu, but after hearing he had a loss of taste, I urged them both to get tested for COVID-19 because testing is the best way for Alaskans to know the true disease burden. I’d told them if Roger needs to go to the hospital for any breathing treatments, having this background test could help expedite that process.
Roger and Jodi were probably irritated with my persistence about getting a COVID-19 test, but they listened. They both tested positive for COVID-19 the 2nd week of November. Jodi had it relatively easy and felt like she has a light cold with some achiness. She recovered quickly. Roger, however, continued to get worse. Jodi is a retired nurse and monitored Roger’s vitals daily, including his O2 stats and blood pressure. She had him lay prone on the bed or with his head below his heart and would cup his back. She contacted his primary care giver to inform her that Roger was sick. He was started on azithromycin. Roger had also been taking elderberry syrup, homemade soups with nutrient dense foods, honey onion cough syrup, Ibuprofen for fever and headache. Roger was so nauseated that he struggled to eat.
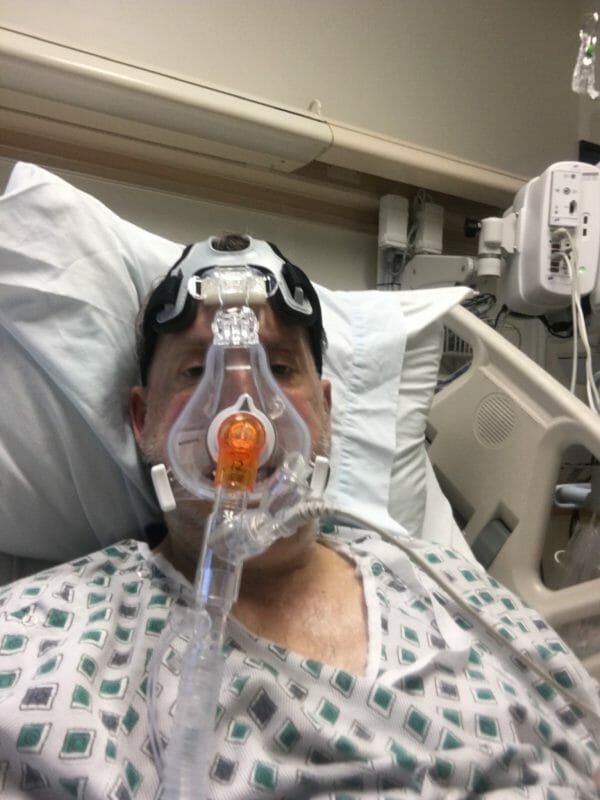
On November 14th, Roger’s O2 dipped below 90 and he went to Central Peninsula Hospital to get checked by a professional. He was admitted for a short time and was given IV Decadron and oxygen. He was sent him home and told to come back if his O2 goes below 90 again. On November 15th he was feeling worse, and Roger was admitted to Central Peninsula Hospital (CPH). His O2 was at 88 and wasn’t recovering. The providers couldn’t get his stats up, but he seemed to be doing ok for a few days and was able to text and call. Over the next few days, he texted less and less until he was only able to “like” our texts to him. His last text to Jodi said “Have I told you I love you, have I told you you’re pretty, have I told you I appreciate you?” This is something he does every day. Jodi texted Roger on one of the quiet days, and a staff person responded. Jodi told that person “I’m praying for him”. The staff person said “I’m praying for him too.”
Around the time he went quiet, he started to use a BiPap–a machine that mechanically assists breathing–at night. Roger kept getting worse and struggled to breathe. On 11/26, Roger was transported to Alaska Regional Hospital to go on a ventilator. They gave him plasma. He had started to get blood clots before BiPap machine in his leg and chest, so he was kept on blood thinners.
Roger stayed on a ventilator for a few weeks, but on December 10th, the staff began to tweak the pressure and O2 flow to see if Roger was making progress. On December 11th, the heavy sedation was turned off. Roger was able to tolerate these changes but was unable to speak and move. It can take time to wake up from propofol sedation. At this point he had COVID Pneumonia, blood clots, brain swelling and lung fibrosis, tachycardia, and heart issues.
Roger had a tracheotomy procedure on December 14th. He’d been on the ventilator for weeks by this point. Tracheostomies can help wean patients off ventilators after long-term use, but it is not always always successful. There are often long-term consequences to being on a ventilator, including infections, and being on long-term sedation can lead to delirium and mental health issues like post-ICU Syndrome (citation: https://www.yalemedicine.org/news/ventilators-covid-19). On December 19th, Roger was transferred to Saint Elias Specialty Hospital. Alaska Regional Hospital had done all they could do for him.
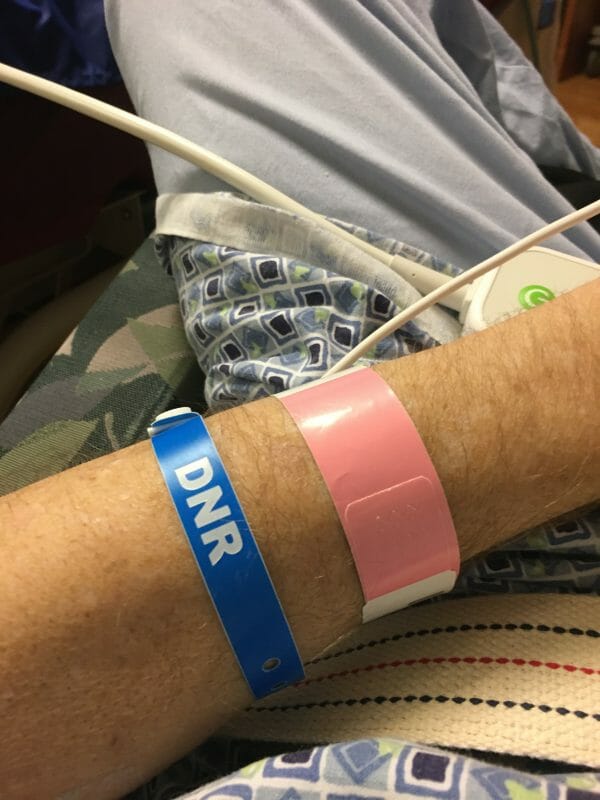
Roger has a foggy memory of the transfer, and remembers it almost like a bad dream. The Propofol caused confusion and some delirium during that transport. He started to go downhill after the transfer and struggled to wake up from his sedation. His blood pressure started to drop, and his other vitals were unstable. On December 21st, his doctor, Dr. Leslie Gonsette, called Jodi to tell her Roger was not doing well. She told Jodi that the lack of elasticity in Roger’s lungs is often seen in patient’s before they pass away. Dr. Gonsette asked whether Roger should be resuscitated if his heart stopped. Jodi answered no. She gave verbal consent for the DNR. Jodi asked “Is he dying? Look. I’ve got to get in there. Our people don’t die alone.” and Dr. Gonsette answered that she understood. The RN later called to tell Jodi she could come in to say goodbye. Jodi took the first plane she could get on from Kenai to Anchorage. She went straight to Saint Elias, was put in full PPE, and was allowed in the room with Roger. Jodi Facetimed me to say my goodbyes. All I could say was “I love you so much, dad” over and over. I didn’t know what else to say to him, I just wanted my dad to know I loved him. He looked so confused and out of it. It was hard to see my strong, capable, vibrant father look so weak and scared. There were so many tubes and IVs in him, and he looked sallow. I will never forget that image.
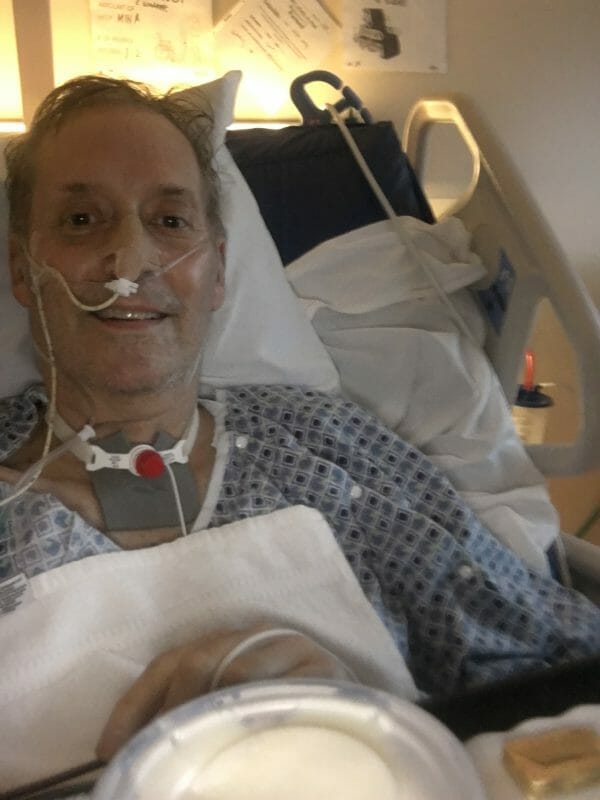
Jodi spent the night praying for him, holding his hand, and being with him. They said the prayer of Salvation. The next morning, Roger started to stabilize. The doctors aren’t sure why that happened, and many have called it a miracle, as that was the only explanation they could come up with. One provider later told us “He had one foot in deaths door and the other foot on a banana peel”. But because he stabilized, Saint Elias staff asked my mom to leave. On 12/24, I received a FaceTime from my dad’s number and wasn’t sure what I’d see when I answered it. By the grace of God and the skills of the medical staff, there was my dad! He was awake, albeit confused, weak, and trying to figure out where he was and what was going on. He thought it was still Thanksgiving and wanted to go home to make the turkey, a tradition he and I have been doing since I was little. He was a bit shocked to learn it was almost Christmas. The Propofol had can cause him to experience delirium and confusion, so he had odd stories about what he thought he’d gone through. He even asked if he’d gone to Montana, Wyoming, or the Caribbean as he had a dream that he was transferred to those different places. This was likely his brain trying to piece together what had happened while he had been sedated.
He was weak, so the call was short, but it was the best Christmas gift I’ve ever received. After that, he began PT/OT with the amazing staff at Saint Elias. I can’t express how amazing the staff at all of the facilities were to my father, from Dr. Gonsette, Dr. Lee, Dr. Caballero, Dr. Shearn, Jean from RT, Ruth from RT, Jen from PT, Shawn from PT, to the nurses, the CNAs, the other OT/PT staff, and many others. I can’t thank them enough for what they did for my family and for their kindness and compassion. Roger would not be here without them. They literally saved his life, and I hope they know how valued they are.
Roger has always been tough and enjoyed sports throughout his life, so naturally, he started pushing himself hard at everything to gain strength and independence. If his PT staff asked him to do a lap around the hall, he’d do two. If they asked him to walk up three steps, he’d do four. He wasn’t going to allow this disease to keep him weak. Severe COVID-19 disease leads to a loss of dignity and autonomy and those things are so important for people. One of Roger’s first big goals was being able to shower by himself and to use the bathroom by himself. He wanted his autonomy back. Roger is about 6’2″ and lost 40-45 lbs while on the ventilator. It was a lot of muscle atrophy from being on the ventilator for so long. He had to relearn how to write, breathe, swallow, walk, etc.
Roger’s original discharge date was set for April 2021, but because of his hard work and improvement it moved up to February 2021. But that wasn’t good enough for my wonderfully stubborn father. He continued to push himself even when his nurses told him to slow down. Sometimes, he’d sneak out of his room with his walker to do extra laps, he was doing extra weight training on his own time, he worked on brain exercises to assess for brain damage, and he refused help with getting from his bed to his chair for meals after he was able to walk himself. Because of this internal drive, he was discharged at the end of January 2021.
When we picked him up at Saint Elias to bring him home, Roger couldn’t get to the car without pausing to breathe and sit. He hyperventilated easily due to severe fibrosis in his lungs (scar tissue). He now has chronic shoulder pain, heart damage, and has clots. This virus leaves people disabled. Roger wasn’t going to let that be his outcome. Today, a man who couldn’t walk a few feet without hyperventilating can now walk for miles each day. He pushed himself to do a short hike with a steep incline recently. He can take care of himself, cook meals, mow the lawn, do household chores, and even drive a car. There is more recovery to do, but Roger has made amazing progress over the last 9 months. Roger was healthy before he got sick, and his providers believe that assisted in his recovery. Many people don’t come off the ventilator, or if they do, they’re stuck on oxygen and don’t have the strength to do the PT/OT work. Roger still does not have his sense of smell or taste fully back yet, though he is slowly starting to taste some foods. One of the greatest things Roger has done since his discharge is providing support to other COVID-19 patients and their families.
As his daughter, this was the hardest thing I have ever been through. I have PTSD and I’m working on it in therapy. Roger also is experiencing anxiety and PTSD. He had no mental health issues prior to being on the ventilator, but it’s common for ICU patients on mechanical ventilation to develop PTSD or other mental health issues. Jodi is dealing with anxiety and likely PTSD, too. It’s not easy to sign a DNR for the person who had been your best friend and spouse for 35+ years.
This happened to us at a time when he wasn’t eligible for a vaccine.
Today there is a vaccine that can prevent severe COVID-19 disease and death, but not enough people are fully vaccinated. Because of this hold out, masking and distancing are important tools to mitigate the spread in our community. My father likely wouldn’t survive a round 2 with COVID-19, so he must be extra cautious; but public health is all of our responsibilities. My family and I are vaccinated, but we still wear masks. I’m forever going to be touched by this virus whether I want to be or not, as is my family and anyone who knows my dad. When people tell me I’m “stupid” or a “sheep” for wearing a mask, I tell them Roger’s story and show them the photos of his struggle.
When someone survives severe COVID-19 disease, it doesn’t end there. There is physical disability that may or may not be permanent. There are mental health repercussions which our state is unfortunately incapable of handling. There is usually organ damage, often to vital organs such as the lungs and heart. There’s survivors’ guilt, too. Roger’s hospitalization and inpatient care bills were over 2 million dollars. He is lucky to have insurance through his time serving in the military with a catastrophic cap, but not everyone has insurance or access to that much money.
We all need to do better to support our communities during this pandemic.
Kaylie Helvie has a Bachelors and Masters degree in Social Work from UAA. She is currently a “Public Health Specialist I” with the state of Alaska in the HIV/STD program. She is writing on behalf of herself and her parents and not on behalf of the state or any organization.



Praise God! We can be “be still and know that we have amazing God! Almighty God! There we are still experiencing Covid 19 season or delta… But we still have the Alpha and Omega. He is beginning and the end. Thank God for a living testimony of God’s healing power like your Dad.To God be the glory!
I’m truly glad your father lived but what is the point of the piece?
Is it a feel good story?
Thanks
The point: get vaccinated.
You are 🍷 ng about the non vaxanated.
Whining? You’ve got a lot of nerve, Richie.
The other point: Have $2 million in health insurance coverage.
This story is to let you know what families go through. And everything that happens. This is a “here what can happen” story. This is a “stay safe and take precautions story.” My uncle survived, when even medical personnel thought he wouldn’t make it. And my cousin wrote this in order to let people know what families go through.
I’m sure both Chris Constant and Felix Revera both had Covid. Reports for restless anal syndrome are on the rise.
Good God, Mr Romero, have you no sense of decency? Devoid of any compassion for someone else’s suffering? With this nasty comment (“restless anal syndrome”), you reveal your true nature.
Wonderful story explaining how we all need to care about each other! Sooo proud of your dad, what a fighter! And praise God! My daughter is an RN with an 8 year old special needs son and has not stopped protecting him. (Wearing a mask and lots of showers) It is so sad that most of the illness and death today from Covid do not need to happen. A tragedy…